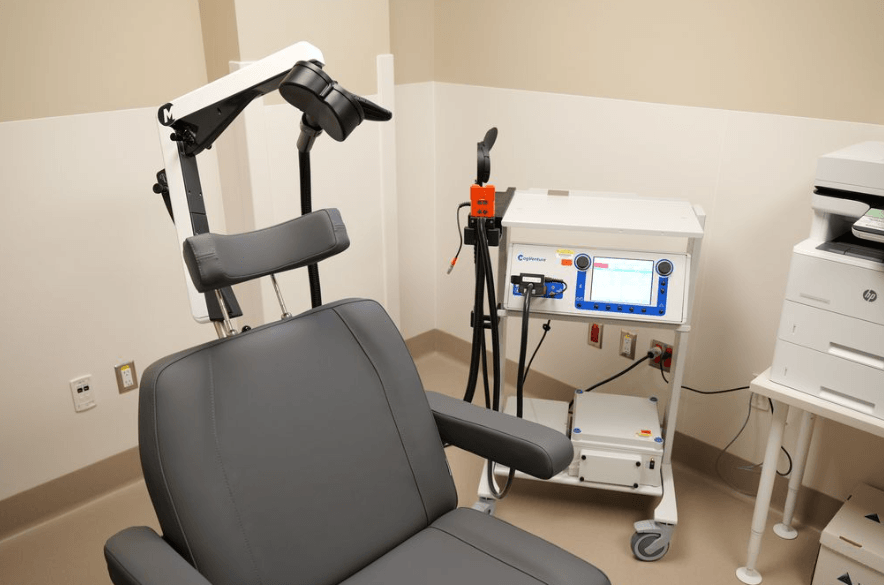
Royal Columbian Hospital Introduces Publicly Funded TMS Therapy for Depression
About one in five Canadians will experience clinical depression during their lifetime, creating growing demand for specialized mental health services across the country. While antidepressant medication and psychotherapy remain common forms of treatment, some patients continue to struggle with symptoms despite multiple interventions.
In response to that need, the Mental Health and Substance Use Wellness Centre at Royal Columbian Hospital has introduced transcranial magnetic stimulation (TMS), a non-invasive treatment designed for people living with treatment-resistant depression.
The program was made possible through funding from the Royal Columbian Hospital Foundation and is now available to eligible adults receiving support through a Fraser Health mental health and substance use program.
Addressing a Growing Need in Mental Health Care
TMS, also known as repetitive transcranial magnetic stimulation, uses magnetic fields to stimulate nerve cells in targeted areas of the brain associated with mood regulation and mental health. During treatment, a magnetic coil is positioned over the patient’s head to deliver controlled pulses intended to improve symptoms of depression.
Mental health professionals at Royal Columbian Hospital say the treatment fills a critical gap for patients who have not benefited from traditional therapies.
“Being able to offer TMS in the public system will improve patient care because there is a huge unmet need for this treatment,” says Dr. Nathan Unger, psychiatrist. “TMS has a really unique place in the treatment algorithm for patients with depression who haven’t responded to multiple medications.”
The introduction of the program reflects broader efforts within Canada’s healthcare system to improve access to advanced mental health treatments as demand for services continues to rise.
Treatment Designed for Outpatient Care
According to hospital officials, the treatment process is designed to minimize disruption to patients’ daily routines. Each appointment lasts approximately 30 minutes, with therapy delivered five days per week over a four- to six-week period. Most patients complete between 20 and 30 sessions.
Healthcare providers say one of the advantages of TMS is its limited recovery time. Side effects are generally minimal, allowing patients to resume regular activities, including driving, immediately following treatment sessions.
“Over four to six weeks, patients may notice improvements in their mood, sleep, appetite and overall functioning,” adds Dr. Unger. “We expect 50 to 60 per cent of patients will experience improvement in their symptoms.”
The treatment is specifically targeted toward adults experiencing treatment-resistant depression, a condition in which patients do not respond adequately to standard antidepressant medications or psychotherapy.
Philanthropy Supporting New Healthcare Technology
Hospital leaders say philanthropic funding played a key role in bringing the treatment program into the public healthcare system.
“This is an example of how philanthropy allows us to work closely with frontline caregivers to identify emerging needs and invest in the tools, training and technologies that support them,” says Royal Columbian Hospital Foundation President and CEO Jeff Norris. “Each year, donors help us fund millions of dollars in equipment, ensuring that our teams can continue to deliver leading-edge care when it matters most.”
Healthcare foundations across Canada have increasingly contributed funding for specialized equipment and emerging technologies as hospitals face pressure to modernize services and expand patient access.
Mental Health Centre Expands Specialized Services
The TMS program forms part of a broader range of mental health and substance use services offered at the Mental Health and Substance Use Wellness Centre, which opened in 2020.
The facility provides both inpatient and outpatient care and includes several specialized programs aimed at supporting patients with diverse mental health needs.
Additional Services Available at the Centre
Current services include:
- A reproductive psychiatry clinic supporting women and families during pregnancy and the post-partum period.
- An Urgent Care Response Centre offering timely mental health assessments without requiring hospital admission.
- Group therapy programs for patients experiencing depression or anxiety.
- A neuropsychology clinic providing specialized cognitive assessments.
- An electroconvulsive therapy clinic.
- Substance use services.
Healthcare providers say expanding access to innovative therapies such as TMS is part of a larger effort to improve long-term mental health outcomes and reduce barriers to care within the public health system.